Scars tell stories of injuries, surgeries, and life experiences, but not everyone wants these permanent reminders visible on their skin. Whether from a medical procedure, accident, or previous cosmetic treatment, unwanted scars can affect confidence and self-image. Fortunately, advancements in dermatological and aesthetic medicine have made surgical scar removal more effective and accessible than ever before. Modern techniques combine precision technology with proven medical protocols to significantly reduce scar visibility, offering renewed hope for those seeking smoother, more uniform skin texture.
Understanding Surgical Scars and Why They Form
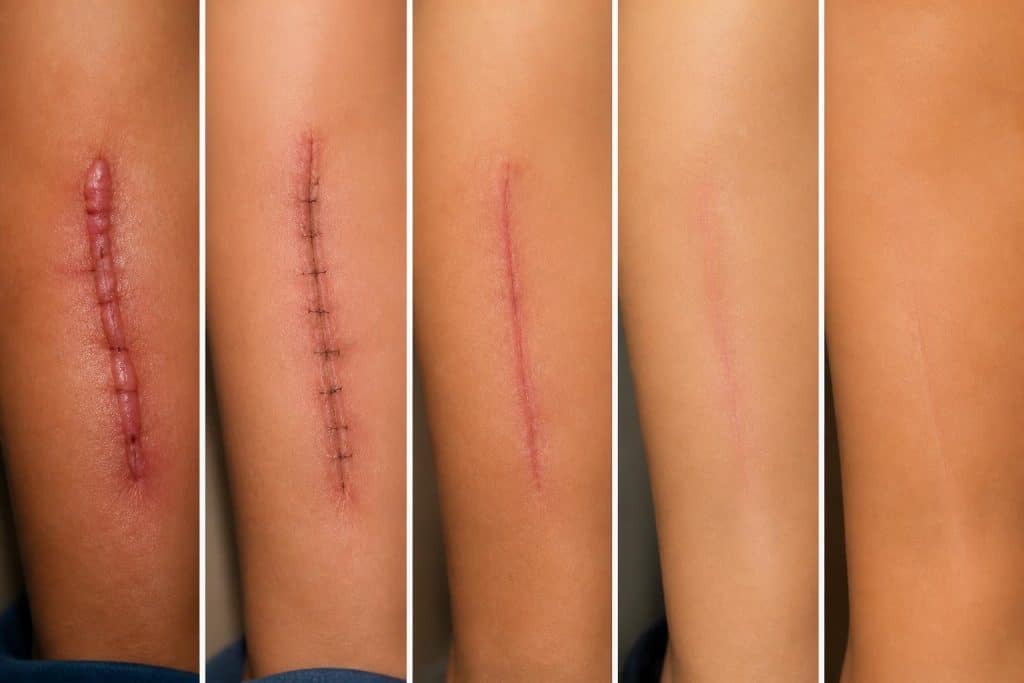
Surgical scars develop as a natural part of the body's healing process following any incision or wound. When skin tissue experiences trauma, the body produces collagen fibers to repair the damage. Unlike the organized pattern of healthy skin, scar tissue forms quickly with a different structural arrangement.
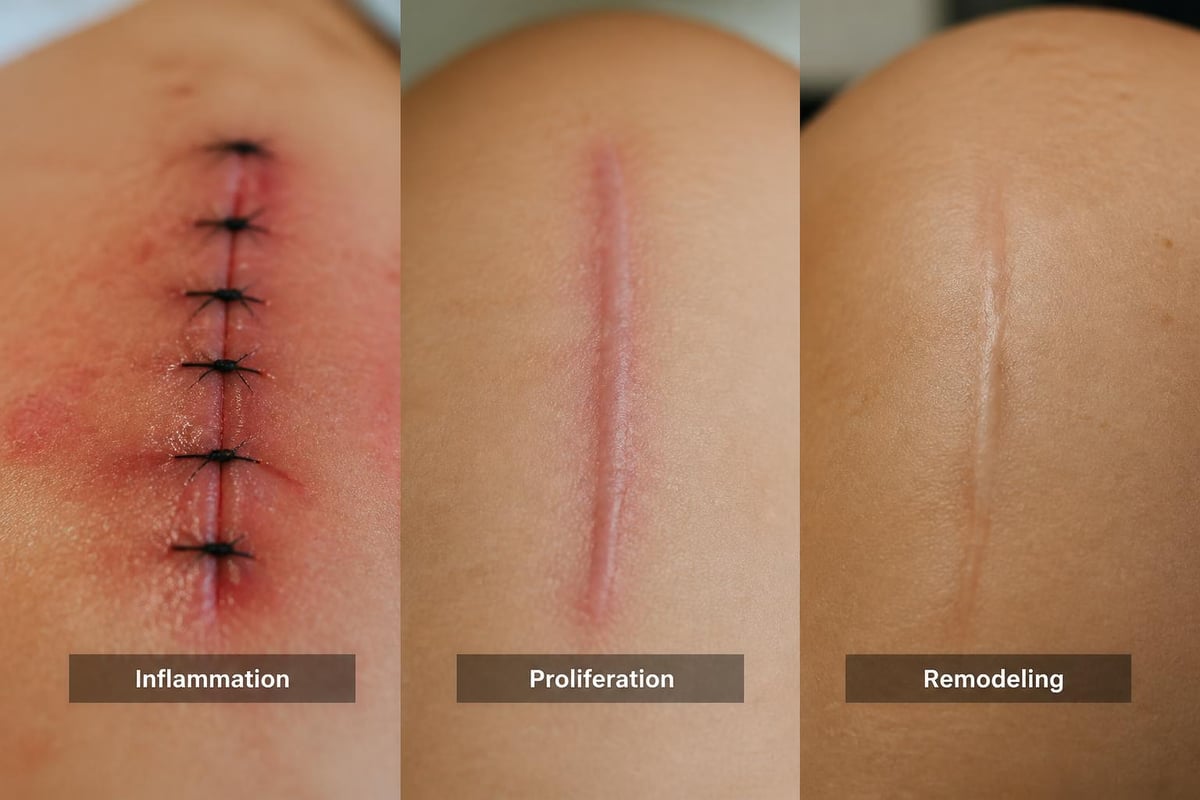
The healing process occurs in three distinct phases:
- Inflammatory phase (days 1-6): Blood clots form, and white blood cells clear debris
- Proliferative phase (days 4-21): Collagen production peaks and new tissue forms
- Maturation phase (21 days to 2 years): Collagen remodels and scars gradually fade
The appearance and severity of surgical scars depend on multiple factors. Genetic predisposition plays a significant role, as some individuals naturally produce more collagen than necessary, leading to hypertrophic or keloid scars. Incision location matters tremendously, with areas under constant tension like shoulders and chest more prone to problematic scarring.
Surgical technique quality also influences outcomes. Clean, precisely closed incisions heal with minimal scarring, while jagged or infected wounds often leave more noticeable marks. Understanding scars and their formation helps patients set realistic expectations for treatment outcomes.
Types of Scars That Benefit From Surgical Removal
Not all scars require intervention, but certain types create functional or aesthetic concerns that warrant treatment consideration. Identifying scar type helps determine the most appropriate surgical scar removal approach.
Hypertrophic Scars
These raised, red scars remain within the original wound boundary but appear thick and elevated. Hypertrophic scars result from excessive collagen production during healing. Unlike keloids, they typically improve over time and respond well to treatment interventions.
Keloid Scars
Keloid scars extend beyond the original injury site, creating raised growths that continue expanding over months or years. More common in darker skin tones, keloids require aggressive treatment and careful monitoring to prevent recurrence. Understanding evidence-based scar management strategies proves essential for addressing these challenging cases.
Atrophic Scars
These depressed scars sit below the surrounding skin surface, commonly resulting from acne, chickenpox, or surgical procedures. The sunken appearance occurs when underlying support structures fail to regenerate properly during healing.
Contracture Scars
Burns often produce contracture scars that tighten skin, potentially restricting movement when they cross joints. These scars require intervention not only for appearance but also to restore function and range of motion.
| Scar Type | Characteristics | Treatment Priority |
|---|---|---|
| Hypertrophic | Raised, within wound boundary | Moderate |
| Keloid | Raised, extends beyond boundary | High |
| Atrophic | Depressed, below surface | Moderate to High |
| Contracture | Tightened, restricts movement | High |
Surgical Scar Removal Techniques and Procedures
Multiple surgical approaches exist for scar removal, each suited to specific scar types and locations. The procedural steps in scar revision vary based on individual patient needs and desired outcomes.
Excision and Re-Closure
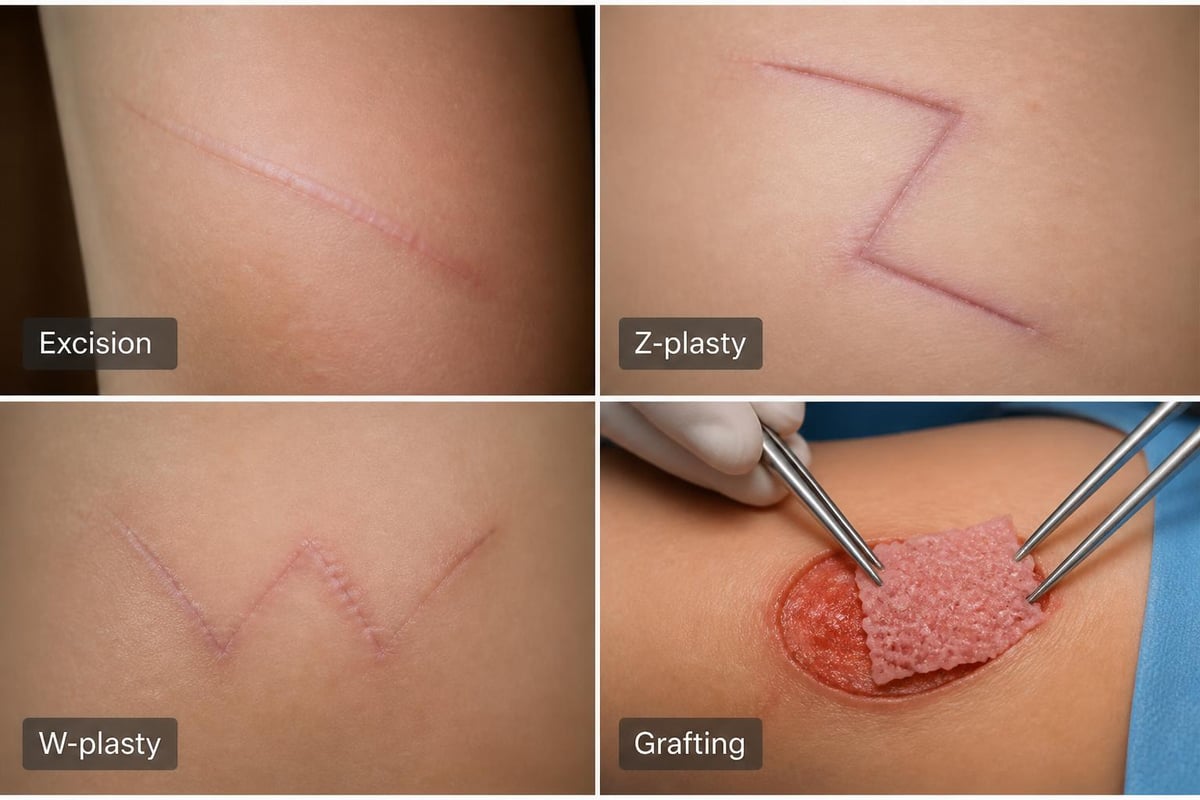
This straightforward approach involves surgically removing the existing scar and meticulously closing the incision using advanced suturing techniques. Surgeons orient new incisions along natural skin lines to minimize visibility. While creating a new scar, the replacement typically heals more favorably than the original.
Excision works best for wide, raised, or irregularly shaped scars. The procedure allows precise control over wound edges and tension, both critical factors in achieving optimal healing.
Z-Plasty and W-Plasty
These specialized techniques reposition scars to align with natural skin creases and contours. Z-plasty creates small triangular flaps that redistribute tension and break up straight scar lines. W-plasty uses irregular patterns to camouflage scars within the skin's natural texture variations.
Both methods prove particularly effective for scars on the face or areas where skin movement creates tension. The geometric patterns help scars blend seamlessly with surrounding tissue.
Skin Grafts and Flaps
Extensive scarring sometimes requires tissue transplantation. Skin grafts transfer skin from donor sites to cover large scarred areas, while flaps move skin along with its blood supply. These complex procedures address severe burns, trauma scars, or cases where local tissue proves insufficient.
Non-Surgical and Minimally Invasive Alternatives
Not every case requires traditional surgical intervention. Modern aesthetic medicine offers several less invasive options that can significantly improve scar appearance, either as standalone treatments or complementary therapies.
Laser therapy represents one of the most advanced approaches available at specialized clinics. Fractional laser systems create microscopic treatment zones that stimulate collagen remodeling without extensive downtime. Different wavelengths target specific scar characteristics, from redness to texture irregularities.
The advanced services at dedicated aesthetic clinics now include multiple laser modalities specifically calibrated for scar improvement. These treatments require multiple sessions spaced several weeks apart for optimal results.
Dermabrasion and Microneedling
Physical resurfacing techniques mechanically remove superficial scar tissue layers. Dermabrasion uses rotating instruments to precisely abrade skin, while microneedling creates controlled micro-injuries that trigger healing responses. Both methods improve texture and stimulate new collagen formation.
Research on surgical scar revision and dermabrasion demonstrates significant improvements in facial scar appearance when these techniques are properly applied.
Injectable Treatments
Corticosteroid injections help flatten raised scars by reducing inflammation and inhibiting excessive collagen production. Dermal fillers address depressed scars by adding volume beneath the skin surface. These minimally invasive options provide temporary to semi-permanent improvements with minimal recovery requirements.
| Treatment Type | Best For | Sessions Needed | Recovery Time |
|---|---|---|---|
| Laser Therapy | Texture, redness, pigmentation | 3-6 | 3-7 days |
| Dermabrasion | Surface irregularities | 1-2 | 7-14 days |
| Steroid Injections | Raised/keloid scars | 2-4 | Minimal |
| Dermal Fillers | Depressed scars | 1-2 | 1-2 days |
The Surgical Scar Removal Recovery Process
Recovery timelines and experiences vary considerably based on the specific procedure performed and individual healing characteristics. Understanding what to expect helps patients prepare mentally and physically for the healing journey.
Immediate post-procedure care focuses on protecting the treatment site and preventing infection. Surgeons typically apply dressings that remain in place for several days, with specific instructions about wound cleaning and moisture management. Avoiding sun exposure proves absolutely critical during early healing stages, as UV radiation can darken scars permanently.
The recovery process following scar revision typically unfolds over several months. Initial healing occurs within two to three weeks, but complete maturation takes six to twelve months. During this time, scars continue improving as collagen remodels and inflammation resolves.
Week-by-Week Recovery Expectations
Weeks 1-2: Swelling, bruising, and redness peak during this period. Sutures may remain in place or require removal depending on location and technique. Activity restrictions prevent tension on healing tissue.
Weeks 3-6: Visible improvements become apparent as inflammation subsides. Patients typically resume normal activities with continued sun protection and scar care protocols.
Months 2-6: Scars continue fading and softening. Texture improvements become increasingly noticeable. Some practitioners recommend silicone sheeting or scar gels during this phase.
Months 6-12: Final results emerge as scars reach full maturity. Most improvements occur by six months, with subtle refinements continuing through the first year.
Pain management remains relatively straightforward for most surgical scar removal procedures. Over-the-counter pain relievers typically suffice, with prescription medications reserved for more extensive interventions. Ice packs and elevation help control swelling during the first week.
Factors Influencing Surgical Scar Removal Success
Multiple variables determine how effectively scars respond to treatment. Understanding these factors helps set realistic expectations and optimize outcomes through proper planning and post-treatment care.
Age significantly impacts healing capacity. Younger patients generally heal faster with more robust collagen production, but this can also increase hypertrophic scar risk. Older patients may experience slower healing but often develop less prominent scars due to reduced collagen density.
Skin tone and type play crucial roles in treatment selection and outcome prediction. Darker skin tones face higher keloid and hyperpigmentation risks, requiring modified approaches and closer monitoring. Fair skin may show redness more prominently during healing phases.
Lifestyle and Health Considerations
- Smoking: Nicotine constricts blood vessels, impairing oxygen delivery to healing tissues
- Nutrition: Protein, vitamin C, and zinc support collagen synthesis and wound healing
- Hydration: Adequate fluid intake maintains skin elasticity and cellular function
- Chronic conditions: Diabetes, autoimmune disorders, and circulation problems complicate healing
Scar location influences both technique selection and outcome potential. Areas under constant tension like shoulders, chest, and joints heal less favorably than relatively stationary regions. Facial scars benefit from abundant blood supply, promoting faster, better healing despite visible location.
The skill and experience of the treating practitioner cannot be overstated. Proper scar revision techniques require meticulous attention to detail, understanding of wound healing biology, and artistic sensibility in tissue handling and closure.

Combining Treatments for Optimal Results
Many patients achieve superior outcomes through strategic combination of surgical and non-surgical approaches. This multi-modal strategy addresses different aspects of scar appearance simultaneously or sequentially.
Surgeons often perform initial excision or revision, followed by laser treatments once primary healing completes. This sequence allows surgical correction of major structural issues while lasers refine texture, color, and residual irregularities. The combined approach produces more comprehensive improvements than either method alone.
Typical combination protocols include:
- Surgical revision to reorient or remove problematic scar tissue
- Four to six week healing period allowing primary wound closure
- Laser therapy series beginning at eight to twelve weeks post-surgery
- Injectable treatments if residual depression or elevation persists
- Ongoing scar care with silicone products and sun protection
Some practitioners integrate treatments during single procedures. For example, dermabrasion might immediately follow surgical excision to blend edges and stimulate collagen remodeling from the start. Injectable steroids sometimes accompany scar excision in keloid-prone patients to suppress excessive healing responses.
Patient compliance with multi-phase treatment plans significantly impacts final results. Completing the full series of recommended interventions, attending follow-up appointments, and maintaining proper scar care between sessions all contribute to success.
Preventing Future Scarring and Maintaining Results
Surgical scar removal represents only part of the journey toward smooth, healthy-looking skin. Protecting improvements and preventing new problematic scars requires ongoing attention and proactive care strategies.
Sun protection stands as the single most important maintenance factor. UV exposure darkens scars, making them more visible even years after treatment. Daily broad-spectrum SPF 30 or higher application to treated areas prevents hyperpigmentation and supports optimal healing.
Silicone-based products demonstrate strong evidence for scar prevention and improvement. Sheets or gels create optimal moisture balance and physical protection that encourages organized collagen formation. Most dermatologists recommend beginning silicone therapy once initial wound closure completes.
Long-Term Scar Care Strategies
Moisture management: Keeping skin properly hydrated prevents excessive dryness that can worsen scar texture and appearance. Quality moisturizers applied twice daily maintain skin barrier function.
Massage therapy: Gentle scar massage after complete healing helps break up adhesions, improve flexibility, and reduce thickness. Using vitamin E or specialized scar oils during massage provides additional benefits.
Activity modification: Avoiding excessive stretching or tension on healing scars during the first six months prevents widening and irregularities. Gradually resuming full activity range allows tissue strength to develop properly.
For individuals undergoing planned surgeries, discussing scar minimization strategies beforehand optimizes outcomes. Selecting experienced surgeons who prioritize aesthetic closure techniques, following pre-operative nutrition and smoking cessation recommendations, and understanding post-operative care requirements all reduce problematic scar risk.
Cost Considerations and Treatment Investment
Financial planning represents a practical reality for anyone considering surgical scar removal. Costs vary substantially based on procedure complexity, geographic location, and practitioner expertise.
Simple scar excisions may cost between $500 and $3,000 per treatment, while complex revisions involving grafts or flaps can exceed $10,000. Laser therapy series typically range from $1,500 to $5,000 depending on scar size and session number required. Injectable treatments fall between $300 and $1,200 per session.
Most insurance plans do not cover purely cosmetic scar treatments. However, scars causing functional impairment, such as contractures limiting movement, may qualify for partial or full coverage. Documentation from treating physicians establishing medical necessity proves essential for insurance consideration.
Many specialized clinics offer financing options or payment plans to make treatments more accessible. Investigating these options early in the consultation process helps patients budget appropriately and avoid financial stress during treatment.
The investment extends beyond monetary considerations. Time commitments for multiple appointments, recovery periods affecting work schedules, and emotional energy required throughout the treatment journey all factor into the overall cost-benefit analysis. Patients should evaluate whether the expected improvements justify these investments based on personal values and priorities.
Selecting the Right Provider for Your Needs
Choosing qualified practitioners significantly influences both safety and aesthetic outcomes. Several credentials and qualifications indicate appropriate expertise for surgical scar removal procedures.
Board certification in dermatology, plastic surgery, or related specialties demonstrates rigorous training and competency standards. These certifications require extensive education, clinical experience, and ongoing professional development to maintain.
Evaluate potential providers based on:
- Years of specific experience with scar revision procedures
- Before-and-after portfolios showing diverse scar types and locations
- Patient reviews and testimonials addressing results and experience quality
- Facility accreditation and safety standards compliance
- Communication style and willingness to address concerns thoroughly
Initial consultations provide opportunities to assess practitioner approach and compatibility. Quality providers conduct comprehensive evaluations, discuss realistic expectations, explain all available options, and outline detailed treatment plans with associated risks and benefits.
Technology availability matters significantly for non-surgical and minimally invasive approaches. Clinics investing in advanced laser systems, precision dermabrasion equipment, and other state-of-the-art devices typically deliver superior results. The commitment to maintaining current technology demonstrates dedication to optimal patient outcomes.
Geographic convenience and ongoing support also deserve consideration. Scar treatment often requires multiple visits over extended periods. Selecting providers with convenient locations and accessible communication channels improves compliance and overall experience quality.
Surgical scar removal in 2026 offers more options and better outcomes than ever before, combining proven surgical techniques with advanced laser and minimally invasive technologies. Whether you're dealing with old surgical scars, injury-related marks, or cosmetic concerns, understanding the available treatments helps you make informed decisions about your skin health journey. New Skin Laser Clinic brings these advanced treatment options to Toronto residents, combining expert estheticians with state-of-the-art technology to create personalized scar treatment plans that deliver real, visible improvements. Schedule a consultation today to discover how modern aesthetic medicine can help you achieve the smooth, confident skin you deserve.